Ο πόνος στο γόνατο μπορεί να μετατρέψει την καθημερινότητα σε έναν διαρκή αγώνα. Απλές δραστηριότητες, όπως το περπάτημα, το ανέβασμα μιας σκάλας ή ακόμα και ο ξεκούραστος ύπνος, γίνονται εξαιρετικά δύσκολες όταν η άρθρωση έχει υποστεί ανεπανόρθωτη φθορά. Όταν η συντηρητική αγωγή, η φυσικοθεραπεία και τα φάρμακα σταματούν να προσφέρουν ανακούφιση, η Ολική Αρθροπλαστική Γόνατος αναδεικνύεται ως η πλέον οριστική και αποτελεσματική λύση.
Στο εξαιρετικά αναλυτικό άρθρο που ακολουθεί, θα εξετάσουμε σε βάθος κάθε πτυχή της ολικής αρθροπλαστικής γόνατος. Θα αναλύσουμε τι ακριβώς είναι, πότε ενδείκνυται, πώς πραγματοποιείται η διαδικασία βήμα προς βήμα, τι πρέπει να περιμένετε πριν και μετά το χειρουργείο, πώς επιτυγχάνεται η ταχύτερη δυνατή αποκατάσταση, αλλά και τις σύγχρονες τεχνικές ελάχιστης επεμβατικότητας (MIS). Παράλληλα, θα αναφερθούμε στον Δρ. Ιωάννη Τσαρούχα, έναν από τους πλέον εξειδικευμένους Ορθοπαιδικούς Χειρουργούς στην Ελλάδα, και στο πώς η εμπειρία του εγγυάται το βέλτιστο αποτέλεσμα.
Η ολική αρθροπλαστική γόνατος είναι μια από τις πιο επιτυχημένες και συχνές ορθοπαιδικές επεμβάσεις παγκοσμίως. Με απλά λόγια, πρόκειται για την αντικατάσταση των φθαρμένων επιφανειών της άρθρωσης του γόνατος (λόγω αρθρίτιδας ή τραυματισμού) με ειδικά τεχνητά εμφυτεύματα, τα οποία ονομάζονται προθέσεις.
Σκοπός της επέμβασης δεν είναι μόνο η εξάλειψη του πόνου, αλλά και η ταυτόχρονη διόρθωση της παραμόρφωσης του γόνατος (όπως το γόνατο που “γέρνει” προς τα μέσα ή προς τα έξω), επιτρέποντας στον ασθενή να ανακτήσει την πλήρη λειτουργικότητα και κινητικότητά του. Τα εμφυτεύματα που χρησιμοποιούνται είναι κατασκευασμένα από κράματα μετάλλων (όπως τιτάνιο ή κοβάλτιο-χρώμιο) και ειδικά πολυμερή (πολυαιθυλένιο), τα οποία είναι απολύτως βιοσυμβατά με το ανθρώπινο σώμα, εξασφαλίζοντας μακροζωία και αντοχή.
Οι σύγχρονες ολικές αρθροπλαστικές διακρίνονται ανάλογα με τον τρόπο σύνδεσης μεταξύ του κνημιαίου και του μηριαίου στοιχείου. Ιστορικά υπήρχαν προθέσεις “τύπου Μεντεσέ” ή “περιοριστικού τύπου”. Σήμερα, ωστόσο, χρησιμοποιούνται κυρίως προθέσεις ημι-περιοριστικού ή μη περιοριστικού τύπου, οι οποίες χαρακτηρίζονται και ως προθέσεις επιφάνειας.
Αυτές οι προθέσεις διακρίνονται περαιτέρω σε:
Η απόφαση για μια ολική αρθροπλαστική γόνατος λαμβάνεται πάντοτε σε συνεργασία με τον ορθοπαιδικό χειρουργό. Η επιτυχής έκβαση του χειρουργείου εξαρτάται σε τεράστιο βαθμό από την ορθή επιλογή του ασθενούς.
Ο ιδανικός υποψήφιος είναι συνήθως ένας ασθενής με:
Σημείωση: Ιδανικός θεωρείται ιστορικά ο λεπτόσωμος ηλικιωμένος ασθενής με περιορισμένη κινητικότητα, ωστόσο με τις σύγχρονες τεχνικές, όλο και περισσότεροι νεότεροι, δραστήριοι ασθενείς υποβάλλονται με απόλυτη επιτυχία στην επέμβαση.
Η επέμβαση δεν πρέπει να πραγματοποιείται (απόλυτες αντενδείξεις) εάν υπάρχει ανεπάρκεια του εκτατικού μηχανισμού του γόνατος, ενεργός σήψη (μικροβιακή λοίμωξη), νευροπαθητική αρθροπάθεια (π.χ. άρθρωση Charcot) ή αν το γόνατο είναι εντελώς “δεμένο” και άκαμπτο λόγω προχωρημένων βλαβών.
Ως σχετικές αντενδείξεις (περιπτώσεις όπου απαιτείται τεράστια προσοχή και αξιολόγηση) θεωρούνται η προηγηθείσα οστεομυελίτιδα στο παρελθόν, η σοβαρή περιφερική αγγειοπάθεια (κακή κυκλοφορία του αίματος στα πόδια) και διάφορες συνοδές σοβαρές παθολογικές καταστάσεις που καθιστούν την αναισθησία επικίνδυνη ή αδύνατη.
Η επιτυχία του χειρουργείου ξεκινά πολύ πριν μπείτε στην κλινική. Η σωστή προετοιμασία μειώνει το άγχος και ελαχιστοποιεί τις πιθανές επιπλοκές.
Πριν την αρθροπλαστική, θα υποβληθείτε σε έναν πλήρη προεγχειρητικό έλεγχο. Αυτός περιλαμβάνει αιματολογικές εξετάσεις, καρδιολογικό έλεγχο (ΗΚΓ, υπέρηχος καρδιάς αν απαιτείται), ακτινογραφία θώρακος και εξειδικευμένες ακτινογραφίες του γόνατος (και συχνά ολόκληρου του ποδιού) για την ψηφιακή προσομοίωση και τον ακριβή υπολογισμό των διαστάσεων των εμφυτευμάτων.
Εάν λαμβάνετε φάρμακα (όπως αντιπηκτικά, ασπιρίνη ή ορισμένα συμπληρώματα), ο γιατρός θα σας δώσει ακριβείς οδηγίες για το πότε πρέπει να τα διακόψετε.
Είναι ζωτικής σημασίας να προετοιμάσετε τον χώρο σας για την επιστροφή σας. Αφαιρέστε χαλιά και καλώδια στα οποία θα μπορούσατε να σκοντάψετε. Τοποθετήστε αντιολισθητικά πατάκια στο μπάνιο και εξασφαλίστε ότι τα αντικείμενα καθημερινής χρήσης (πιάτα, ρούχα, φάρμακα) βρίσκονται σε εύκολα προσβάσιμο ύψος, ώστε να μην χρειάζεται να σκύβετε ή να τεντώνεστε έντονα τις πρώτες ημέρες.
Πώς ακριβώς διενεργείται μια ολική αρθροπλαστική γόνατος; Ας δούμε την ενδελεχή χειρουργική διαδικασία, η οποία απαιτεί τεράστια μηχανική ακρίβεια και ορθοπαιδική δεξιοτεχνία.
Παραδοσιακά, η εγχειρητική τομή γινόταν στην πρόσθια επιφάνεια και έφτανε τα 20-25 εκατοστά. Σήμερα, τα πράγματα έχουν αλλάξει ριζικά. Η προσπέλαση γίνεται μέσω μιας μέσης ή παράμεσης τομής. Η άρθρωση ανοίγεται “έσω παρεπιγονατιδικά” με ελάχιστη επέκταση υπέρ-επιγονατιδικά, προσπαθώντας ο χειρουργός να σεβαστεί τις ίνες του τετρακέφαλου μυός και να μην τις κόψει άσκοπα.
Ένα από τα σημαντικότερα βήματα. Εάν το γόνατό σας είναι “στραβό” (προεγχειρητική ραιβότητα ή βλαισότητα), αυτό πρέπει να διορθωθεί απολύτως. Αν παραμείνει παραμόρφωση, τα υλικά θα φορτίζονται ασύμμετρα και θα χαλαρώσουν γρήγορα. Για να επιτευχθεί η ευθυγράμμιση, η οστεοτομία (το κόψιμο του φθαρμένου οστού) της κνήμης γίνεται αυστηρά κάθετα στον επιμήκη άξονα της κνήμης, ενώ το κάτω πέρας του μηριαίου κόβεται σε συγκεκριμένες μοίρες. Στόχος είναι ο μηχανικός (εκτατικός) άξονας να περνά ακριβώς από το κέντρο της άρθρωσης (το μεσοσπονδύλιο έπαρμα της κνήμης).
Η σταθερότητα της νέας άρθρωσης δεν εξαρτάται μόνο από τα μέταλλα, αλλά κυρίως από τα μαλακά μόρια (συνδέσμους). Ο χειρουργός πρέπει να εξασφαλίσει ισόρροπη τάση των πλάγιων συνδέσμων σε όλο το εύρος της κίνησης. Αυτό επιτυγχάνεται δημιουργώντας ένα απολύτως ίσο κενό όταν το γόνατο είναι λυγισμένο (Flexion Gap) και όταν είναι τεντωμένο (Extension Gap). Εάν υπάρχει ανισορροπία, εφαρμόζεται προσεκτική “απελευθέρωση” (release) των μαλακών μορίων στην πλευρά που “τραβάει” περισσότερο.
Οι προθέσεις (τα τεχνητά μεταλλικά καπάκια που ντύνουν το μηριαίο και την κνήμη) δεν μπαίνουν τυχαία. Στο μετωπιαίο επίπεδο, πρέπει να τοποθετούνται έτσι ώστε ο μηχανικός άξονας να είναι άριστος. Στο προσθιοπίσθιο επίπεδο, η κνημιαία πρόθεση πρέπει συχνά να έχει μια ελαφριά οπίσθια κλίση 3-7 μοιρών για να επιτρέπει καλή κάμψη. Στη μηριαία πρόθεση απαγορεύεται αυστηρά η υπερέκταση, καθώς μπορεί να οδηγήσει σε κάταγμα, ενώ πρέπει να αποφεύγεται η εσωτερική ή εξωτερική στροφή για να λειτουργεί σωστά ο τετρακέφαλος.
Τέλος, ελέγχεται η “κύλιση της επιγονατίδας”. Η επιγονατίδα (το καπάκι του γόνατος) πρέπει διεγχειρητικά να κυλά ομαλά μέσα στη νέα μεταλλική αύλακα του μηριαίου. Αν δεν το κάνει, απαιτείται μικρή χειρουργική απελευθέρωση των έξω καθεκτικών συνδέσμων της.
Η στερέωση των προθέσεων στο οστό μπορεί να γίνει με χρήση ειδικού ακρυλικού “τσιμέντου” (οστικό τσιμέντο) ή χωρίς τσιμέντο (press-fit). Η χρήση τσιμέντου παραμένει η μέθοδος εκλογής (gold standard) και υπερτερεί στις περισσότερες περιπτώσεις, εξασφαλίζοντας άμεση σταθερότητα. Η μέθοδος χωρίς τσιμέντο επιλέγεται συχνά σε νεότερους ασθενείς με εξαιρετικά δυνατό, σκληρό οστικό υπόστρωμα, ώστε το κόκκαλο να αναπτυχθεί μέσα στους πόρους του μετάλλου.
Ανάμεσα στα μεταλλικά στοιχεία παρεμβάλλεται ένα πλαστικό ένθετο: το πολυαιθυλένιο. Αυτό λειτουργεί ως ο νέος “χόνδρος”. Για να επιβιώσει η αρθροπλαστική για δεκαετίες χωρίς να φθαρεί το πολυαιθυλένιο (γεγονός που θα προκαλούσε φλεγμονή και χαλάρωση), πρέπει να δέχεται συμμετρικές πιέσεις. Οι σύγχρονες τεχνικές επιτάσσουν το πολυαιθυλένιο να έχει πάχος τουλάχιστον 8-10 χιλιοστά και να διαθέτει μεγάλη επιφάνεια επαφής με τους μηριαίους κονδύλους.
Τα τελευταία χρόνια, η μέθοδος M.I.S. (Minimally Invasive Surgery) έχει φέρει επανάσταση στην ολική αρθροπλαστική γόνατος. Τι ακριβώς προσφέρει και γιατί υπερτερεί;
Στην M.I.S., χρησιμοποιούνται ειδικά, μικροσκοπικά εργαλεία. Τα πλεονεκτήματα είναι εντυπωσιακά:
Συνδυαστικά με συστήματα Ρομποτικής υποβοήθησης ή ψηφιακής πλοήγησης, ο χειρουργός έχει την ικανότητα να τοποθετήσει τα υλικά με ακρίβεια χιλιοστού και μοίρας (τρισδιάστατη όραση, 35% λιγότερη αφαίρεση οστού), προσαρμόζοντάς τα απόλυτα στο “ψηφιακό αποτύπωμα” της ανατομίας του κάθε ανθρώπου.
Μόλις ολοκληρωθεί η επέμβαση, θα μεταφερθείτε στον θάλαμο ανάρρωσης. Χάρη στα σύγχρονα αναισθησιολογικά πρωτόκολλα (συνήθως ραχιαία αναισθησία σε συνδυασμό με τοπική έγχυση αναλγητικών μιγμάτων γύρω από το γόνατο – LIA), ο πόνος είναι απολύτως ελεγχόμενος. Ξεχάστε τις εποχές όπου η αρθροπλαστική συνοδευόταν από αφόρητους πόνους. Σήμερα, η έμφαση δίνεται στην αναλγησία.
Όπως προαναφέρθηκε, θα σας ζητηθεί (και θα σας βοηθήσουν) να κάνετε τα πρώτα σας βήματα μέσα στο δωμάτιο την ίδια κιόλας μέρα, χρησιμοποιώντας ένα περιπατητήρα (Π). Η πρώιμη κινητοποίηση αποτελεί το “κλειδί” για την αποφυγή επιπλοκών όπως οι θρομβώσεις και για την ταχύτερη ανάνηψη των μυών.
Η επιτυχία της επέμβασης ανήκει κατά 50% στον χειρουργό και κατά 50% στον ίδιο τον ασθενή και το πρόγραμμα φυσικοθεραπείας του. Η αποκατάσταση είναι μια διαδικασία που απαιτεί υπομονή και συνέπεια.
Τις πρώτες ημέρες, συχνά χρησιμοποιείται ένα ειδικό μηχάνημα συνεχούς παθητικής κίνησης (CPM – Continuous Passive Motion). Ενώ εσείς αναπαύεστε στο κρεβάτι, το μηχάνημα λυγίζει και τεντώνει το γόνατό σας αργά και ανώδυνα. Αυτό αποτρέπει τον σχηματισμό συμφύσεων (ουλώδους ιστού) που θα μπορούσαν να προκαλέσουν δυσκαμψία. Στόχος του χειρουργού είναι το μετεγχειρητικό εύρος κίνησης του γόνατος να φτάσει τουλάχιστον από τις 0 μοίρες (πλήρης έκταση) έως τις 110 μοίρες (ικανοποιητική κάμψη), κάτι που επαρκεί για σχεδόν όλες τις καθημερινές δραστηριότητες (οδήγηση, σκαλοπάτια, κάθισμα).
Η συνεισφορά των φυσικοθεραπευτών είναι καθοριστική. Το πρόγραμμα ξεκινά άμεσα και περιλαμβάνει:
Κάθε χειρουργική επέμβαση ενέχει κινδύνους, όμως στην ολική αρθροπλαστική γόνατος (ειδικά με τις σύγχρονες MIS τεχνικές), τα ποσοστά επιπλοκών είναι εξαιρετικά χαμηλά:
Όπως τονίζουν οι ειδικοί, τυχόν παρατήρηση συμπτωμάτων (έντονο πρήξιμο στη γάμπα, πυρετός, ξαφνικός πόνος) στο σπίτι, πρέπει να αναφέρεται άμεσα στον θεράποντα ιατρό.
Η επιλογή του σωστού ορθοπαιδικού χειρουργού είναι η πιο κρίσιμη απόφαση για μια επιτυχημένη αρθροπλαστική. Ο Dr. Ioannis Tsarouchas, γεννημένος στην Καρδίτσα, είναι ένας καταξιωμένος επιστήμονας με τεράστια κλινική και χειρουργική εμπειρία.
Είναι Διδάκτωρ του Πανεπιστημίου Αθηνών (από το 1999) και σήμερα κατέχει τη θέση του Διευθυντή της Ορθοπαιδικής Κλινικής Μεγάλων Αρθρώσεων στο Ιατρικό Κέντρο Αθηνών. Η πορεία του περιλαμβάνει τη Διεύθυνση της Α’ Ορθοπαιδικής Κλινικής στο νοσοκομείο Ερρίκος Ντυνάν για πάνω από μια δεκαετία, ενώ η εξειδίκευσή του ξεκίνησε από την Πανεπιστημιακή Κλινική του Νοσοκομείου ΚΑΤ.
Ο Δρ. Τσαρούχας θεωρείται πρωτοπόρος σε τεχνικές ελάχιστης επεμβατικότητας (MIS). Εκτός από την εξειδίκευσή του στις πρωτοπαθείς και ρομποτικές ολικές αρθροπλαστικές γόνατος (και τις δύσκολες αναθεωρήσεις αυτών), είναι από τους κορυφαίους χειρουργούς στην Ελλάδα στη μέθοδο ASI (Anterior Supine Intermuscular) για την αρθροπλαστική του ισχίου. Διατηρεί συνεχή επιστημονική παρουσία, με ομιλίες και ανακοινώσεις στα μεγαλύτερα συνέδρια, διασφαλίζοντας ότι οι ασθενείς του λαμβάνουν πάντοτε την πιο σύγχρονη, ασφαλή και εξατομικευμένη θεραπεία. Μέλημά του είναι πάντα η λεπτομερής ενημέρωση, η άρτια χειρουργική πράξη και η ανθρώπινη προσέγγιση σε κάθε περιστατικό.
Για να καλύψουμε πλήρως τις απορίες σας, συγκεντρώσαμε τις πιο συχνές ερωτήσεις γύρω από την επέμβαση:
Με τη χρήση σύγχρονων υλικών (ισχυρά κράματα τιτανίου/κοβαλτίου) και εξαιρετικά ανθεκτικού πολυαιθυλενίου μεγάλου πάχους (8-10 χιλιοστών), αλλά και χάρη στην τέλεια μηχανική ευθυγράμμιση (ρομποτική / MIS πλοήγηση), υπολογίζεται ότι οι σημερινές προθέσεις αντέχουν 15 έως 20 χρόνια, και σε πολλές περιπτώσεις εφ’ όρου ζωής του ασθενούς. Το “κλειδί” είναι η αποφυγή υπερβολικής τριβής και συμμετρικής φόρτισης, γι’ αυτό και ο ορθοπαιδικός μετρά κάθε χιλιοστό της επέμβασης.
Χάρη στα σύγχρονα αναισθησιολογικά πρωτόκολλα (Fast Track), τα εξειδικευμένα αναλγητικά (block νεύρων, LIA), και τον μηδενικό τραυματισμό των μυών (λόγω MIS), ο μετεγχειρητικός πόνος είναι απολύτως ελεγχόμενος και ήπιος. Η αίσθηση παρομοιάζεται περισσότερο με μετεγχειρητικό “πιάσιμο” και βάρος, παρά με οξύ πόνο.
Σε ορισμένες περιπτώσεις, εφόσον ο ασθενής είναι υγιής, σε καλή βιολογική ηλικία και δεν έχει σοβαρά καρδιολογικά ή αναπνευστικά προβλήματα, μπορεί να πραγματοποιηθεί ταυτόχρονη αντικατάσταση και των δύο γονάτων, μειώνοντας τον συνολικό χρόνο αποκατάστασης. Αυτό, ωστόσο, αποφασίζεται αυστηρά και μόνο μετά από πλήρη ιατρικό έλεγχο από τον ορθοπαιδικό και τον αναισθησιολόγο.
Ναι. Η φυσικοθεραπεία στο σπίτι για τις πρώτες εβδομάδες είναι απαραίτητη. Θα μάθετε πώς να περπατάτε σωστά, πώς να ανεβοκατεβαίνετε σκάλες (ανεβαίνουμε με το “καλό” πόδι, κατεβαίνουμε με το “χειρουργημένο”) και πώς να ενδυναμώσετε τους μύες του ποδιού σας.
Τα μεταλλικά στοιχεία της πρόθεσης ενδέχεται να ενεργοποιήσουν τους ανιχνευτές μετάλλων στα αεροδρόμια. Συνήθως αρκεί να αναφέρετε στο προσωπικό ασφαλείας ότι φέρετε τεχνητή άρθρωση. Ο ιατρός σας μπορεί να σας παρέχει και μια σχετική βεβαίωση, αν και συνήθως ο λεκτικός έλεγχος και τα σύγχρονα σκάνερ αρκούν.
Η Ολική Αρθροπλαστική Γόνατος δεν είναι απλώς μια χειρουργική επέμβαση. Είναι μια επένδυση στην ποιότητα ζωής. Για τους ανθρώπους που υποφέρουν καθημερινά από τις επιπτώσεις της προχωρημένης οστεοαρθρίτιδας, η δυνατότητα να περπατήσουν ξανά χωρίς πόνο, να ταξιδέψουν, να παίξουν με τα εγγόνια τους ή να επιστρέψουν σε αγαπημένες συνήθειες, φαντάζει συχνά σαν θαύμα.
Σήμερα, με την εφαρμογή τεχνικών ελάχιστης επεμβατικότητας, τη χρήση ρομποτικής υποβοήθησης και τα εξατομικευμένα πρωτόκολλα αποκατάστασης, η διαδικασία έχει γίνει ταχύτερη, ασφαλέστερη και απείρως πιο ανώδυνη από ό,τι στο παρελθόν. Υπό την καθοδήγηση ενός εξειδικευμένου και έμπειρου χειρουργού, όπως ο Dr. Ioannis Tsarouchas, η επιστροφή σε μια φυσιολογική καθημερινότητα δεν αποτελεί απλώς μια ελπίδα, αλλά μια ιατρική βεβαιότητα. Εάν ο πόνος στο γόνατο σας κρατάει πίσω, ίσως ήρθε η ώρα να κάνετε το βήμα για να διεκδικήσετε και πάλι τη ζωή σας.
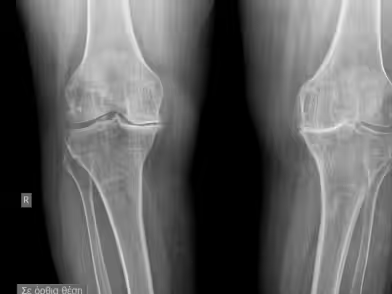
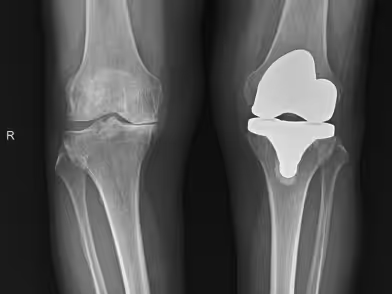
Depending on the connection between the femoral and tibial components, prostheses may be hinge or constrained, semi-constrained, or non-constrained (surface replacement). The latter are most commonly used today and can be classified as cruciate-retaining, posterior-stabilized (substituting for the posterior cruciate ligament), or posterior cruciate-sacrificing designs.
There is no clear advantage between different surface replacement designs. Prosthesis fixation may be cemented or cementless. Cemented fixation tends to yield better outcomes, whereas cementless fixation is recommended for younger patients with excellent bone stock. Polyethylene quality and thickness are crucial for implant longevity. It must be loaded symmetrically, provide a wide contact surface with the femoral condyles to minimize pressure, and be at least 8–10 mm thick. Range of motion should reach 0–110 degrees. Early movement may begin with a Continuous Passive Motion (CPM) machine, followed by supervised physiotherapy.
Infection occurs in 1–2% of cases, thromboembolism in 0.5–2%, and neurovascular injury in 0.05%, along with risks of blood loss and wound problems. However, in recent years, minimally invasive (MIS) techniques, have significantly reduced these complications, allowing faster patient mobilization with less soft tissue damage and fewer surgical risks.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)