The loosening of a total arthroplasty may be attributed either to mechanical factors or to infection. Common causes include aseptic loosening, periprosthetic infection, acute or chronic polyethylene wear, patellar complications, knee instability, and periprosthetic fractures.
The principles of revision surgery are similar to those of primary arthroplasty. However, the revision surgeon is faced with additional challenges such as bone loss, ligamentous instability, and joint line alteration.
Preoperative evaluation: A thorough history, including details regarding the type of pain before and after the initial operation, can be useful for diagnosis.
Clinical assessment: It is essential to exclude other potential causes of knee pain. The hip must also be evaluated, as well as possible vascular pathologies. Radicular symptoms from the spine should be ruled out, as well as conditions such as diabetic neuropathy.
The knee itself should be examined for joint effusion, increased temperature, and reduced range of motion.
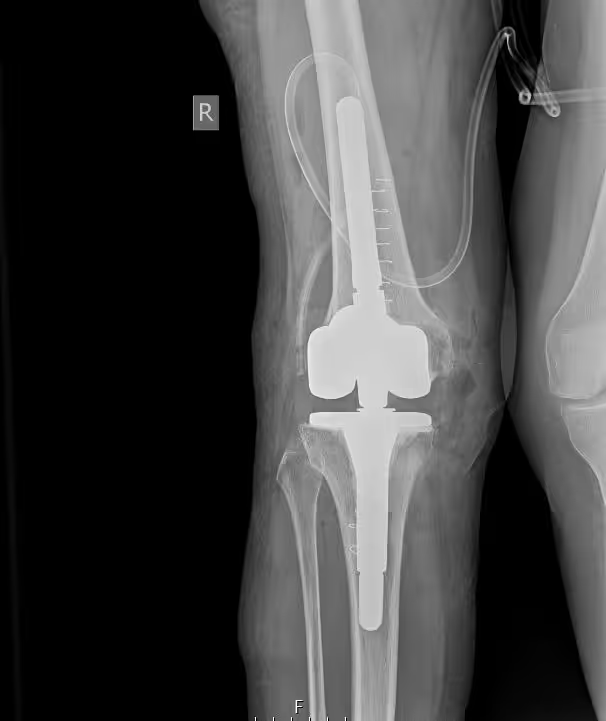
Radiological evaluation: Plain radiographs are mandatory, as they may reveal radiolucent lines and areas of bone loss.
Bone scintigraphy: In cases where radiographs are inconclusive, a bone scan may demonstrate increased uptake, suggesting loosening.
Laboratory tests: Beyond routine blood tests, ESR and C-reactive protein levels must be assessed, as they are indicators of infection.

Stop living in pain, improve the quality of your life!
The main challenges during revision for aseptic loosening are scar tissue from the previous surgery and bone loss. With the development of new prosthetic designs and improved surgical techniques, long-term outcomes are favorable, with survival rates exceeding 80% at ten years.
Patella: In most cases, patellar resurfacing is not deemed necessary during the initial operation. Problems are more common when the patella is replaced, particularly if maltracking occurs in the femoral component’s trochlea, which may require surgical correction of the retinacular ligaments.
Periprosthetic fracture: These are more frequent when a notch is created in the anterior femoral cortex during insertion of the femoral component. Management is difficult due to compromised bone quality and the presence of the prosthesis. If the prosthesis remains stable, a retrograde intramedullary nail may be a good option. If loosening is present, revision with a new prosthesis is indicated.
Periprosthetic joint infection represents one of the most challenging complications due to the thin soft tissue envelope and limited potential for extensive surgical debridement. In these cases, revision total knee arthroplasty is usually performed in two stages: First, the removal of all components, extensive surgical debridement, and placement of an antibiotic-loaded cement spacer to maintain joint space.
The re-implantation of the new prosthesis after six to eight weeks, provided that infection markers have normalized. Some authors advocate for single-stage revision in selected cases (particularly with Gram-positive organisms), but this approach is generally considered aggressive.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)