

The hip joint is one of the largest and most important joints in the human body, as it connects the trunk to the lower limb. It consists of the acetabulum (the articular surface of the pelvis), the femoral head, and the surrounding soft tissues (synovial membrane, joint capsule, ligaments). The articulating surfaces of the acetabulum and femoral head are covered with articular cartilage, a special, smooth, and resilient tissue that allows smooth movement with minimal friction.
Osteoarthritis is a chronic degenerative joint disease in which the articular cartilage gradually deteriorates. The loss of cartilage leads to abnormal movement between the femoral head and acetabulum, the formation of osteophytes (bony spurs in areas where bone does not normally exist), and, in advanced stages, direct bone-on-bone contact with destructive consequences for the articulating bones.
Hip osteoarthritis is estimated to affect about 10–20% of the population (approximately 90 per 100,000 per year). It usually appears after the age of 50, more frequently in women (especially in Southern Europe), and is less common in individuals of African descent.
Causes are varied and include age-related wear, previous injuries, congenital hip dysplasia, increased body weight, repetitive stress (due to occupation or sports), and hereditary predisposition.
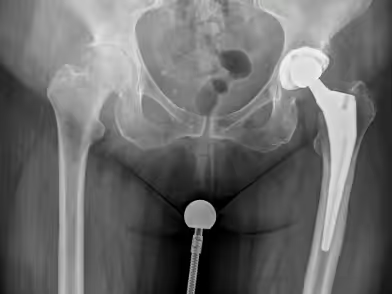
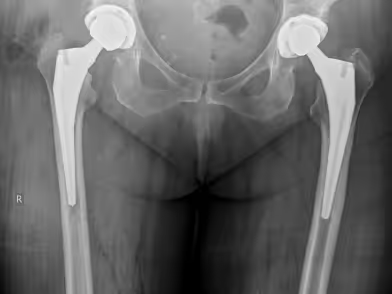
Pain is the main symptom of the disease. It is typically located in the groin and may radiate to the ipsilateral knee or buttock. In the early stages, pain occurs after exertion, but later it may appear even at rest. Patients may have difficulty climbing stairs or walking, especially on uneven ground.
Stiffness or a sensation of “locking” of the joint appears in later stages. Patients find it difficult to bring the thigh towards the abdomen and have restricted internal and external hip rotation. Combined with pain, this limits daily activities, such as putting on socks and shoes or trimming toenails. Stiffness may be worse after rest and improve with a few steps.
Patients often present with limping (antalgic gait), either due to pain or because joint destruction has led to shortening of the affected limb and leg length discrepancy. The affected leg is often shorter, sometimes by more than two centimeters.
Many patients with hip osteoarthritis also suffer from low back pain, either due to leg length discrepancy or antalgic gait.
A. Clinical examination
Diagnosis of hip osteoarthritis can be made by clinical assessment, taking into account the patient’s history (symptoms, age, occupation, activities, prior injuries, comorbidities, medications, family history) and clinical tests. Pain on hip rotation when the thigh is flexed towards the abdomen is the most common finding. Pain may also occur during hip adduction or abduction, with decreased range of motion, or with flexion contracture (persistent mild hip flexion preventing full extension).
Β. Imaging
A plain anteroposterior (AP) pelvic X-ray in standing position is the primary diagnostic tool. Main findings include:
In rare cases where plain radiographs do not confirm the diagnosis (e.g., early stages without significant structural damage), CT or MRI may be necessary.

Stop living in pain, improve the quality of your life!
Α. Conservative treatment
In the early stages of hip osteoarthritis, treatment is conservative and includes:
Β. Surgical Treatment - ASI method
The definitive treatment for hip osteoarthritis is total hip arthroplasty, i.e., replacement of the joint with an artificial one.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)