

Hip dysplasia in adults is the result of abnormal joint development from birth, persisting into adult life, and resulting in a shallow, underdeveloped acetabulum and a defective proximal femur. Specifically, developmental dysplasia of the hip (DDH) is the most common orthopedic condition in newborns, with an incidence of 1 in 100 live births, while congenital hip dislocation occurs in approximately 1 in 1,000. The disease encompasses a spectrum ranging from simple dysplasia (a shallow, hypoplastic acetabulum) to subluxation (partial loss of contact between the femoral head and acetabulum) and finally to dislocation, where there is complete loss of contact between the articular surfaces and central migration of the femur. The prevalence of adult hip dysplasia in the United States is estimated to be 3–5%, and approximately 10% of all total hip arthroplasties are performed due to secondary arthritis resulting from hip dysplasia. Women are two to four times more likely to develop hip dysplasia compared to men. Other risk factors include breech presentation, oligohydramnios, being the firstborn, improper swaddling, and a positive family history.
While adult hip dysplasia almost exclusively requires surgical treatment to improve function and relieve symptoms, developmental dysplasia of the hip in newborns and infants—the primary form of the condition—can be diagnosed as early as the second month of life. At that stage, it can be successfully managed in nearly 90% of cases with specialized braces or casts. For this reason, neonatal screening with clinical examination, and, depending on national guidelines, hip ultrasound, is of great value.
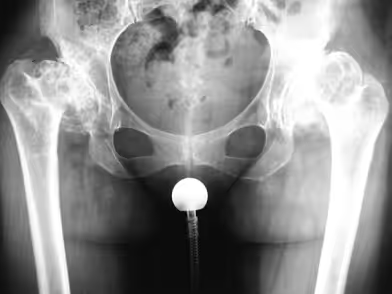
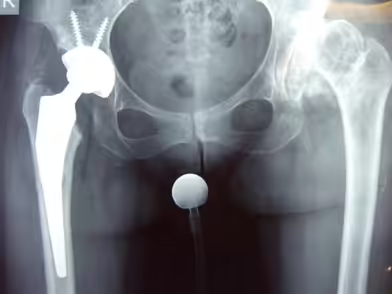
Both bony and soft tissue deformities associated with hip dysplasia result in abnormal femoral head motion within the acetabulum. This abnormal loading leads to excessive stress on the acetabular rim, resulting in cartilage damage and the gradual development of secondary osteoarthritis. Anatomical abnormalities include a shallow acetabulum with varying degrees of deficiency of the superior and lateral walls, sometimes accompanied by a pseudoacetabulum. Femoral deformities may also be present, including excessive femoral neck anteversion, head-neck junction deformities, coxa valga, hypoplasia of the femoral canal, and posterior displacement of the greater trochanter.

Stop living in pain, improve the quality of your life!
Two main classification systems are used. The Hartofilakidis classification recognizes three types: Type A (dysplasia): the femoral head remains contained within the acetabulum but in a subluxated position. Type B (low dislocation): the femoral head is dislocated and articulates with a pseudoacetabulum located just superior to the true acetabulum. Type C (high dislocation): the femoral head is completely dislocated and has migrated to a more central and posterior position relative to the true acetabulum. The Crowe classification, on the other hand, categorizes dysplasia into four grades based on the degree of proximal migration/subluxation of the femoral head, expressed as a percentage of pelvic height or femoral head diameter.
Clinically, patients with hip dysplasia most commonly present with hip or groin pain, often of sudden onset and aggravated by hip flexion and internal rotation. Lateral hip pain may also be caused by trochanteric bursitis. Some patients demonstrate an antalgic gait due to hip abductor weakness or fatigue. Clinical examination assesses posture, gait, and generalized ligamentous laxity. Findings may include increased external rotation due to femoral anteversion, pain during active or passive hip flexion and rotation, and positive provocation tests (e.g., anterior instability test or prone external rotation test), indicative of joint instability.
Plain radiographs (anteroposterior, lateral, and false profile views) are the most commonly used diagnostic tools. Various radiographic parameters can assist in diagnosis and classification. CT is usually reserved for preoperative planning, assessing acetabular and proximal femoral morphology, and femoral anteversion.
While conservative treatment may be considered for selected patients with minimal symptoms, long-term non-operative management is not recommended, as secondary hip osteoarthritis develops early in the disease course. Joint-preserving surgeries are indicated for adolescents and young adults with congruent hips, a nearly normal range of motion, and no established osteoarthritis. The procedure of choice is periacetabular osteotomy (PAO), which reorients the acetabulum through controlled osteotomies of the supporting pelvic bones. This improves femoral head coverage without disrupting the external rotators. Patients are usually allowed protected weight-bearing postoperatively. The main goal is to restore bony coverage of the femoral head, thereby delaying or preventing the need for total hip arthroplasty. International literature reports up to 92% success in avoiding hip replacement following PAO.
Pelvic osteotomies may also be combined with femoral osteotomies when intraoperative hip flexion beyond 90° and internal rotation beyond 15° cannot be achieved, to prevent femoroacetabular impingement and associated labral or cartilage damage. Hip arthroscopy may be considered in selected cases, typically in mild dysplasia or following PAO, to address labral tears, chondral lesions, or cam-type deformities. However, arthroscopy alone in moderate-to-severe dysplasia is associated with high failure and reoperation rates.
In patients with non-congruent hips and inadequate femoral head coverage, salvage osteotomies such as the Chiari or Shelf procedures have been used with relative success to delay end-stage osteoarthritis. When advanced osteoarthritis has developed, total hip arthroplasty (THA) remains the treatment of choice, reliably relieving pain and improving function. However, THA in dysplastic hips is technically more challenging and carries a higher risk of complications compared to THA for primary osteoarthritis. Although minimally invasive approaches are generally avoided, in our clinic, the Anterior Supine Intermuscular (ASI) approach is routinely performed even in dysplastic hips. Hip resurfacing arthroplasty has also been described in dysplastic hips, offering more bone preservation of the femoral head and neck. However, given the high prevalence of proximal femoral deformities in these patients, its use should be highly selective to avoid excessive complication rates.
Adult hip dysplasia is an uncommon but clinically significant condition representing the natural progression of developmental dysplasia of the hip in adolescents and young adults. Prevention through neonatal screening is of paramount importance both for patients and healthcare systems. Nevertheless, adult hip dysplasia can be effectively managed with a range of surgical techniques—from joint-preserving procedures to total hip arthroplasty—ultimately leading to improved functional outcomes.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)