Definition
Osteonecrosis – bone necrosis – occurs either due to obstruction of the blood flow to the bone or to extensive destruction of the bone marrow and bone cells.
Localized bone necrosis is a characteristic feature of various conditions such as epiphyseal inflammation, fractures and dislocations, decompression sickness in divers, Gaucher disease, alcohol abuse, sickle cell anemia, vasculitis, and long-term use of high-dose corticosteroids.
Knee osteonecrosis is most often encountered in individuals over the age of 50–60, predominantly in women (ratio 3:1), and its onset is usually sudden. It typically affects the medial femoral condyle of the knee.
Clinical presentation
The early stage of bone necrosis is asymptomatic, and when symptoms finally appear, the disease has usually already progressed significantly.
Pain is the most common symptom. More specifically, it presents suddenly, is more intense at night, and is felt around the joint, mainly at the medial femoral condyle. Mild synovitis and limitation of the range of motion are usually present. Some patients also complain of a sensation of catching or a clicking sound, which may be due to impingement or entrapment from a loose cartilaginous fragment. In advanced stages, the knee joint becomes stiff and deformed.
Diagnostic Methods
Plain radiographs may become useful a few weeks after the infarction, showing either subchondral sclerosis, diffuse sclerosis, or a thin diagonal fracture line just beneath the articular surface, usually of the medial femoral condyle (face, profile, tunnel view).
In the early stages of the disease, only bone scintigraphy and MRI can reveal ischemic lesions in the marrow, long before plain radiographs show abnormalities.

Stop living in pain, improve the quality of your life!
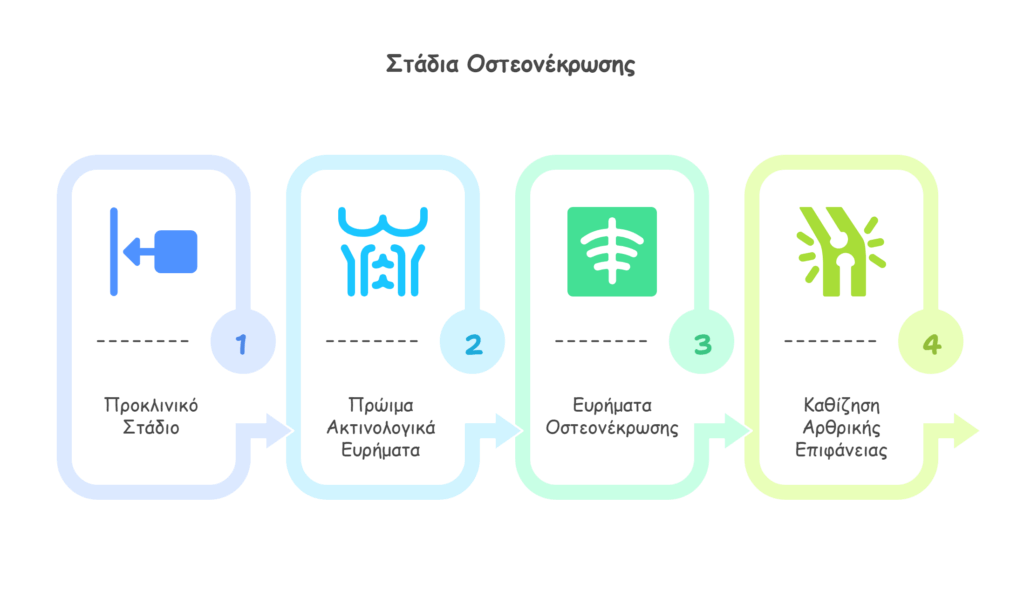
Stage 1: Preclinical stage of ischemia and early necrosis without radiographic changes. Only MRI can reveal early bone marrow abnormalities.
Stage 2: Painful stage with early radiographic findings but nearly normal bone contours.
Stage 3: Radiographic signs of osteonecrosis with abnormal bone contours.
Stage 4: Collapse of the articular surface and secondary degenerative osteoarthritis changes.
Diagnosis
In most cases of knee osteonecrosis, the underlying cause is typically revealed through a thorough medical history. Possible etiologies include trauma, deep-water diving, sickle cell anemia, a history of high-dose corticosteroid use, and alcohol abuse.
Prognosis
The prognosis depends greatly on the size of the lesion. If the total affected area is less than 3.5 cm² and involves less than 30% of the medial femoral condyle surface, spontaneous healing is often possible.
Larger lesions, however, are likely to progress.
Treatment
In the early stages, unloading of the affected limb may provide some benefit.
With disease progression, treatment becomes surgical. Depending on the stage and patient’s age, options include microfracture, core decompression (drilling), or, in larger lesions, autologous chondrocyte transplantation (mosaicplasty). In end-stage osteonecrosis, surgical management includes unloading osteotomy, unicompartmental knee arthroplasty, or total knee arthroplasty.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)