

However, as with any prosthesis, revision total hip arthroplasty may be subject to various types of mechanical or biological failure. Such a failure may necessitate a second surgery to address the issue. This repeat surgery is referred to as a revision hip.
The majority of patients who undergo revision total hip arthroplasty retain their prosthesis for 15 to 20 years, sometimes even for life. However, some patients may require one or more revision surgeries, particularly if the initial operation was performed at a younger age and the patient leads a very active lifestyle.
Preoperative examinations for patients undergoing revision are more extensive compared to those for primary surgery. Specialized radiographs, CT scans, or MRI may be required to assess implant orientation and identify possible causes of bone loss around the prosthesis. If infection is suspected, a preoperative aspiration or specialized blood tests may be necessary.
Main Reasons for Revision Hip Surgery:
In Europe, approximately 18 revision procedures are performed for every 100 primary hip arthroplasties. The most common reasons include:
The prosthesis mimics the structure of the natural hip joint, forming a ball-and-socket articulation. For the prosthesis to function properly, the femoral component must remain securely within the acetabular component. Proper orientation of both components, as well as muscle and ligament support around the joint, is essential in preventing dislocation.
Although hip revision is designed to allow a wide range of motion, trauma or certain joint positions may force the femoral component out of the socket, leading to hip dislocation.
Dislocations are relatively rare, particularly in healthy patients who follow their surgeon’s postoperative instructions. However, certain groups, such as elderly patients with comorbidities or those who underwent hip replacement after a fracture or multiple prior surgeries, are more predisposed.
Once a first dislocation occurs, the risk of recurrence increases significantly, as the event disrupts surrounding muscles and ligaments. Multiple dislocations, though uncommon, may occur and can necessitate revision surgery. In some cases, surgeons may use a constrained socket to limit the risk of further dislocation.
Proper soft-tissue healing after revision is crucial for surgical success, and bracing may be recommended for a few weeks. Following the surgeon’s instructions and avoiding high-risk movements is essential.

Stop living in pain, improve the quality of your life!
During hip motion, the femoral and acetabular components move against one another, gradually causing wear. The younger and more active the patient, the faster this process occurs. Repeated motion may lead to small fragments breaking off the implant, which can be plastic, cement, ceramic, or metal, depending on the prosthesis. The immune system recognizes these particles as foreign bodies, triggering an inflammatory response. A strong reaction may cause osteolysis (bone destruction around the implant). Severe osteolysis increases the risk of implant loosening.
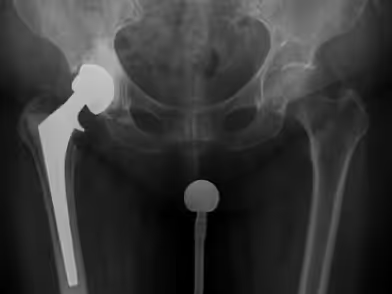
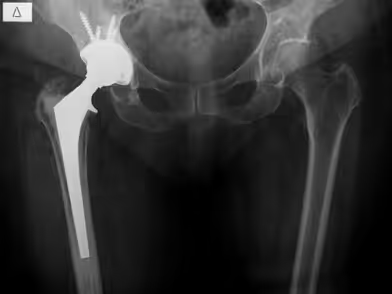
A periprosthetic infection may occur at any time after surgery, with the risk being highest within the first six weeks. Later infections are less common. Bacteria from infections elsewhere in the body (e.g., oral cavity, lungs, urinary tract, or skin) may enter the bloodstream and settle around the implant, forming a biofilm that supports bacterial growth and causes hip pain and fever.
If periprosthetic infection is suspected, the surgeon will identify the microorganism responsible while starting empirical antibiotics. Aspiration of the hip joint and microbiological analysis of the fluid help determine the bacterial type and antibiotic sensitivity.
Once confirmed, treatment options vary, most involving surgery combined with targeted antibiotics. The approach depends on bacterial strain, infection duration, implant fixation status, and overall patient health.
Surgical options include:
Patients should be informed about postoperative complications such as implant wear, periprosthetic infection, and dislocation, which can often be prevented by following medical advice. Prophylactic antibiotics before dental procedures, for example, can reduce infection risk.
Since wear and osteolysis may progress silently without pain, regular follow-up with clinical exams and radiographs is critical. If excessive wear or osteolysis is detected, revision may be required.
During revision, the surgeon may remove or replace one or more components of the prosthesis. Non-fixed parts can be replaced with little or no bone removal, but revision of components integrated with bone may cause bone loss. Surrounding muscles may also be affected, reducing hip strength and function.
The outcomes of revision are less predictable compared to primary hip arthroplasty, with higher complication rates. Revision surgery is longer, more complex, and technically demanding. For this reason, such procedures should be performed by highly experienced surgeons in hospitals with advanced facilities.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)