Hip Arthroplasty - Rehabilitation


Total hip arthroplasty is one of the most frequently performed orthopedic procedures. The first attempts to replace the arthritic surfaces of the hip joint date to the 1890s, and since then, progress has been remarkable regarding surgical approaches and techniques, available instruments, implants, biomaterials, and more. Modern total hip arthroplasty is based on the principles of low-friction arthroplasty, as first described and implemented by Sir John Charnley in the 1960s. Today, it is considered one of the most successful orthopedic operations in our field. The main indication for total hip arthroplasty is end-stage hip arthritis. The etiology may be unknown (primary arthritis) or secondary to another condition leading to joint destruction, such as intracapsular hip fractures (femoral neck or subcapital fractures), certain fractures of the femoral head or acetabulum, osteonecrosis (avascular necrosis) of the femoral head, hip dysplasia, crystal-induced or rheumatoid arthritis, septic arthritis, neoplastic diseases, etc.
Hemiarthroplasty of the hip, on the other hand, involves the implantation of a femoral stem either with or without cement, and in most cases a bipolar prosthetic head. This consists of a small metallic head enclosed within a larger metallic shell, functioning as a single unit. In this technique, the acetabular surface is not replaced, allowing the prosthetic head to articulate directly with the native acetabulum. In contrast, the two components of the prosthetic head slide and rotate synchronously within it.
Total and Hemiarthroplasty of the Hip
There are two main categories of hip arthroplasty: total and hemiarthroplasty. Total hip arthroplasty consists of replacing both the acetabular and femoral articular surfaces with prosthetic components, along with the insertion of a bearing surface (liner). Together with the prosthetic femoral head, these components are designed to ensure optimal tribological conditions for joint movement. The most commonly used type of total hip arthroplasty includes a metallic acetabular component with either a polyethylene or ceramic liner, and a metallic femoral stem with a metallic or ceramic prosthetic head. Today, implant fixation is most often achieved with cementless (press-fit) techniques, sometimes supported with screws for acetabular stability. Cemented fixation is also possible or even preferable in certain cases, such as in severely osteoporotic bone or after radiotherapy. Other options in total hip arthroplasty include dual mobility implants or even constrained liners.
Before
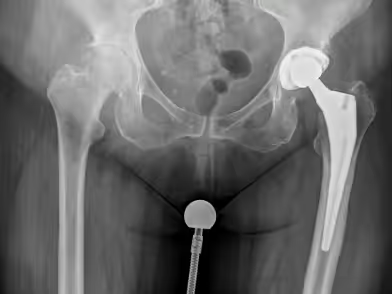
After
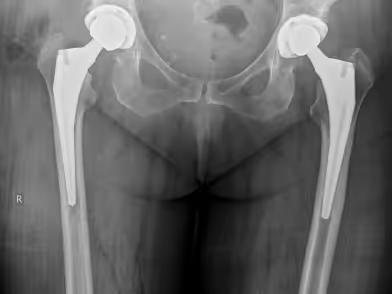
Preoperative Evaluation and Planning
Routine preoperative assessment of patients scheduled for total hip arthroplasty includes, in addition to history-taking and clinical examination, anteroposterior pelvic radiographs in the standing position (if possible), as well as lateral hip views. It is also good practice to obtain radiographs of the ipsilateral femur, particularly in cases of previous orthopedic surgeries further down the limb. Basic laboratory tests, an electrocardiogram, a chest X-ray, and pre-anesthetic assessment are also performed, along with consultation from a cardiologist or other specialists if required. Moreover, the surgical team evaluates the preoperative radiographs to estimate implant sizes and positioning, leg length discrepancy and its correction, and other technical details. Patients are informed about the potential need for blood transfusion intra- or postoperatively, and are asked to review and sign the informed consent form with the guidance and support of the surgical team.

Stop living in pain, improve the quality of your life!
Surgical Procedure of Hip Arthroplasty
During surgery, the patient is positioned either supine or lateral decubitus, depending on the surgeon’s preferred approach to the hip joint. The surgical field is sterilized to cover a wide area, including the abdomen up to the umbilicus and either the operative leg alone or both legs down to the ankle. After creating a sterile surgical field with drapes, a skin incision is made, its location depending on the chosen approach. The approach also determines which soft tissues (muscles, tendons, joint capsule, etc.) must be detached to access the hip joint.
From that point, the surgical steps are similar regardless of approach. The femoral neck is cut at a predetermined level using a saw, and the femoral head is removed. The acetabulum is then prepared with hemispherical reamers to the appropriate size, and a trial cup is inserted to assess stability. Once stable and fully seated, the final acetabular component is implanted press-fit, with the trial liner inside. Attention is then directed to the femur, whose canal is opened and progressively reamed and rasped to accommodate the smallest rasp. Using rasps of increasing size, the femur is prepared until the final rasp is fully seated and rotationally stable. With a trial neck and head, the hip is reduced and evaluated for range of motion, stability, impingement, and leg length discrepancy. Intraoperative radiographic control of the prosthesis is recommended at this stage. Once all conditions are met, the joint is dislocated again, and the final implants are placed: the liner, the femoral stem, and the prosthetic head. After final reduction, the surgical wound is irrigated, and local anesthetic and tranexamic acid are injected for pain and bleeding control. Finally, the wound is closed in layers, ensuring restoration of all disrupted anatomical structures.
Postoperative Rehabilitation
During the immediate (in-hospital) postoperative period following routine hip arthroplasty, patients begin full weight-bearing ambulation with the aid of a walker or two crutches. Graduated compression stockings and oral or subcutaneous anticoagulation are used for 40 days postoperatively, while perioperative antibiotic prophylaxis is also administered. Pain control is achieved initially with intravenous analgesics, followed by oral medications upon discharge, typically including paracetamol and a mild opioid (e.g., codeine or tramadol), along with an anti-inflammatory drug.
Depending on the surgeon’s protocol, patients may or may not be prescribed postoperative physiotherapy sessions. When prescribed, these focus on gait training with aids (walker or crutches) indoors and outdoors, stair climbing, entering and exiting a car, and progressive mobilization and strengthening exercises involving the trunk, hip, and knee. Patients must also understand and strictly follow hip precautions during the first 4–6 postoperative weeks to avoid dislocation. Regardless of surgical approach, these precautions include avoiding hip flexion beyond 90 degrees in any position (standing, lying, or sitting). Depending on the approach used, additional restrictions apply: avoiding adduction and internal rotation (e.g., turning the foot inward, lying on the side without a pillow between the thighs) for posterior approaches, or avoiding abduction and external rotation (e.g., sitting cross-legged) for lateral and anterolateral approaches. Ultimately, return to full weight-bearing without aids and driving is expected within 4–6 weeks postoperatively, at which time a follow-up clinical and radiographic evaluation is scheduled. Most patients undergoing total hip arthroplasty for arthritis will eventually “forget” they ever had hip surgery, while returning to most low- and moderate-impact sports is considered safe.
Hip arthroplasty today is considered a routine orthopedic procedure that has successfully relieved the symptoms of thousands of patients suffering from hip arthritis and other conditions. Although it can be performed using various surgical approaches, the underlying rationale remains the same, and studies have demonstrated equally satisfactory long-term functional outcomes regardless of approach. Modern postoperative rehabilitation protocols emphasize immediate and at least partial, if not full, weight-bearing after surgery, as well as faster return to daily activities, work, and sports.
READ RECENTLY
CONTACT
Contact the doctor
to guide you about your condition, so you can choose the best possible treatment for it.
