The prosthetic components must be well-aligned to ensure reduced friction between them, allowing for an unrestricted range of motion. At the same time, during wound closure, it is essential to respect the surrounding soft tissues, as they contribute to the stability of the prosthetic joint.
There are essentially three variations of shoulder arthroplasty: Shoulder Hemiarthroplasty (HA), where only the articular surface of the humeral head is replaced with a prosthetic implant. Anatomic Total Shoulder Arthroplasty (TSA): both the glenoid and humeral head are replaced with prostheses that replicate the original curvature of the joint surfaces. Reverse Shoulder Arthroplasty (RSA): both joint surfaces are replaced with prostheses of opposite curvature compared to the native anatomy.
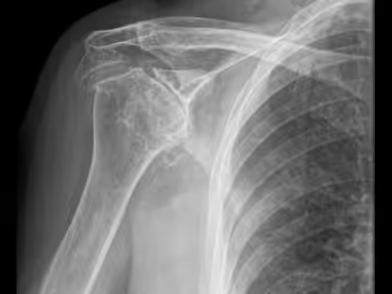
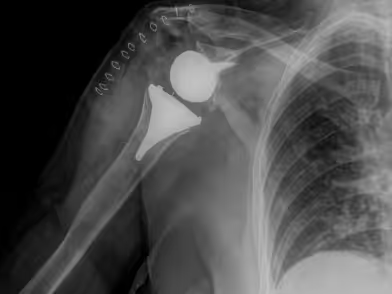
The choice among these types depends primarily on the biological age of the patient, the condition of the rotator cuff muscles and tendon integrity, as well as the exact indication for shoulder arthroplasty. Anatomic TSA is generally indicated for primary and secondary osteoarthritis of the shoulder, provided there is sufficient glenoid bone stock, intact and functional rotator cuff and deltoid muscles, a fully functional brachial plexus, no superior migration of the humeral head (which would suggest cuff tear arthropathy), and no evidence of active infection. Shoulder hemiarthroplasty is indicated for cases of primary arthritis with rotator cuff deficiency or inadequate glenoid bone stock, as well as in younger, physically active patients due to the higher risk of glenoid component loosening. It is also used in selected cases of cuff tear arthropathy, osteonecrosis of the humeral head without glenoid involvement, certain 3-part and most 4-part proximal humeral fractures, and nearly all intra-articular fractures of the humeral head in patients younger than 65–70 years. Reverse Shoulder Arthroplasty is indicated for older patients with cuff tear arthropathy, shoulder osteoarthritis with irreparable cuff tears, 3- and 4-part proximal humeral fractures, intra-articular fractures of the humeral head in patients over 70 years or with severe osteopenia, rheumatoid arthritis of the shoulder (if sufficient glenoid bone stock exists), and after failed hemiarthroplasty or anatomic TSA. A functional deltoid muscle is crucial for the success of RSA.

Stop living in pain, improve the quality of your life!
Shoulder arthroplasty is most often performed under general anesthesia, sometimes supplemented with regional nerve blocks (interscalene or supraclavicular) for postoperative pain management. In selected cases, when general anesthesia is contraindicated, regional anesthesia techniques can be used to allow the procedure. The patient is positioned in a semi-reclined "beach-chair" position, and the surgical field is prepared and draped. All three variations of shoulder arthroplasty are traditionally performed through a deltopectoral approach, with an incision starting below the acromion and extending distally, lateral to the axillary fold, following the interval between the deltoid and pectoralis major. Access to the joint is gained by detaching the subscapularis insertion and opening the capsule, or in fractures by following fracture fragments and attached rotator cuff tendons. An alternative anterosuperior approach can also be used, preserving the subscapularis by mobilizing the anterior deltoid insertion. The humeral head is osteotomized at the anatomic neck, unless already fractured. For hemiarthroplasty, only the humerus is prepared to receive a prosthesis (with or without cement) consisting of a stem and head. For TSA and RSA, the glenoid must also be prepared. In TSA, a cemented all-polyethylene concave glenoid component is implanted; in RSA, a press-fit baseplate with a central peg and screws is implanted, onto which a convex glenosphere is attached. In TSA, the humeral component is similar to that of hemiarthroplasty. In RSA, the humeral component consists of a stem with a concave surface that articulates with the glenosphere. The implants are secured, followed by reattachment of the subscapularis tendon or fracture fragments carrying cuff tendons to the humerus or stem using non-absorbable sutures. Standard layered closure is performed, usually without drains, and a bulky dressing is applied. The arm is then immobilized in a shoulder brace.
Rehabilitation depends on fracture presence and subscapularis repair. Fractures require 6–8 weeks of protected passive mobilization until healing. Subscapularis repair requires restriction of active internal rotation and passive external rotation for 6 weeks. Pushing up from a chair with the operated arm is strictly prohibited during this period. In most other cases, a simple sling is used for comfort for 3 weeks. Early on, gentle scapular motion and distal joint exercises (elbow, forearm, wrist, hand) are allowed. After immobilization, assisted and passive shoulder mobilization begins, followed by active range of motion and progressive strengthening. Most patients regain full daily function within 2–3 months, while heavy laborers typically return to full work in 4–6 months.
Complications of shoulder arthroplasty can be divided into general complications with symptoms such as infection, deep vein thrombosis, neurovascular injury, stiffness and reduced range of motion, aseptic loosening of the humeral component, failed subscapularis repair with anterior instability (anterior dislocation), malunion or non-union of tuberosities, and periprosthetic fracture (intra- or postoperative). Procedure-specific complications with symptoms such as glenoid loosening in TSA, glenoid loosening and notching or acromial insufficiency fracture in RSA, and anterior-superior escape in HA. Although the list appears extensive, most are uncommon, and numerous measures are taken to prevent, detect, and manage them promptly.
In conclusion, shoulder Arthroplasty is a surgical technique that can treat a wide range of shoulder pathologies, from advanced rotator cuff insufficiency to osteoarthritis. Depending on the indication, it may take the form of hemiarthroplasty, anatomic total shoulder arthroplasty, or reverse total shoulder arthroplasty. Success depends largely on patient selection, making it a critical factor in optimizing long-term outcomes. With proper indications and technique, shoulder arthroplasty can reliably provide pain relief and functional improvement for a wide range of patients.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)