
Shoulder osteoarthritis may be classified as primary (of unknown cause) or secondary, due to various pathological conditions such as post-traumatic arthritis, post-dislocation arthritis, inflammatory and crystal arthropathies, osteonecrosis, neuropathic arthritis (Charcot joint), and rotator cuff arthropathy.
Post-traumatic arthritis usually develops when irregularities form on the joint surface after a fracture. Similarly, post-dislocation arthritis can occur as a result of cartilage damage that may arise even after a single dislocation episode. Another cause is rotator cuff arthropathy, which develops when large or massive tears in the rotator cuff lead to progressive insufficiency. This insufficiency allows the humeral head to migrate upward, eventually impinging against the acromion and causing cartilage wear. Osteonecrosis is another condition that can lead to joint degeneration. It occurs when the blood supply to the humeral head is disrupted, either by traumatic causes such as fractures or dislocations, or by non-traumatic factors including long-term corticosteroid use, alcoholism, or bone marrow disorders. The loss of blood flow results in cell death, collapse of the subchondral bone, and ultimately degeneration of the cartilage. Finally, inflammatory and crystal arthropathies contribute to progressive joint damage through different mechanisms. Inflammatory causes are typically linked to systemic autoimmune diseases, such as rheumatoid arthritis, while crystal arthropathies result from the deposition of uric acid or other salts within the joint surfaces.
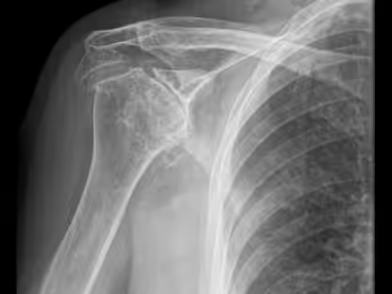
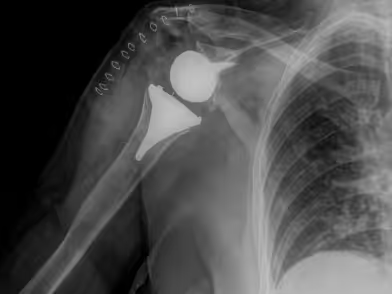
Patients with shoulder osteoarthritis often present with activity-related pain that persists at rest, along with reduced range of motion, particularly external rotation. Some patients may be unable to actively abduct the shoulder, a clinical sign known as pseudoparalysis, due to advanced rotator cuff insufficiency. Sleep may gradually become more difficult, either because of pain itself or due to difficulty finding a comfortable position. In addition, crepitus (audible or palpable joint noises from intra-articular structures) may occur during motion.
Initial imaging includes plain radiographs, which usually suffice to demonstrate joint surface degeneration and additional bony changes. CT scans and MRI can be employed for preoperative evaluation—CT to assess glenoid morphology and MRI to assess the rotator cuff muscles and tendons.

Stop living in pain, improve the quality of your life!
The management of shoulder osteoarthritis involves both conservative and surgical approaches. In most cases, treatment begins conservatively with the use of paracetamol or non-steroidal anti-inflammatory drugs (NSAIDs) to control pain, combined with physiotherapy aimed at improving joint mobility and muscle strength. Intra-articular injections that mix a local anesthetic with corticosteroids can also be used to provide temporary relief from pain and inflammation, although their effect is usually short- to medium-term. When the underlying cause of the condition is inflammatory, it is important to consult a rheumatologist, since disease-modifying therapies may significantly change the progression of the disease.
Surgical treatment for shoulder osteoarthritis is chosen based on the severity of the disease and the condition of the surrounding structures. In mild-to-moderate cases where conservative measures are no longer effective, arthroscopic debridement can be performed to delay the need for joint replacement. In younger patients, this procedure may also involve removing hypertrophic synovium, osteophytes, loose bodies, and releasing the joint capsule, an approach collectively known as Comprehensive Arthroscopic Management (CAM). When joint replacement becomes necessary, the choice of procedure depends largely on the integrity of the rotator cuff and deltoid muscles. If both remain intact, an anatomic total shoulder arthroplasty (TSA) is usually preferred. However, if the rotator cuff is deficient but the deltoid is still functional, a reverse shoulder arthroplasty (RSA) offers the best outcome. In selected cases, such as younger patients with osteonecrosis or rheumatoid arthritis where the glenoid bone stock is inadequate, a hemiarthroplasty may be considered. In very rare and severe situations—such as persistent infection, nerve paralysis, major soft-tissue insufficiency, or recurrent instability after previous surgeries—the only viable option may be shoulder arthrodesis. While this procedure eliminates shoulder movement, it stabilizes the joint in a functional position so that the patient can still use the arm effectively.
Similar to other major joints of the human body, shoulder osteoarthritis is a painful and limiting condition that affects many individuals. While its causes vary, it is less common than knee or hip osteoarthritis. Diagnosis is relatively straightforward, and treatment options range from conservative to surgical interventions. The most appropriate approach should always be tailored to the patient’s specific condition.
to guide you about your condition, so you can choose the best possible treatment for it.
We use cookies to improve your experience on our site. By using our site, you consent to cookies.
Manage your cookie preferences below:
Essential cookies enable basic functions and are necessary for the proper function of the website.
These cookies are needed for adding comments on this website.
Google reCAPTCHA helps protect websites from spam and abuse by verifying user interactions through challenges.
Google Tag Manager simplifies the management of marketing tags on your website without code changes.
Marketing cookies are used to follow visitors to websites. The intention is to show ads that are relevant and engaging to the individual user.
Google Maps is a web mapping service providing satellite imagery, real-time navigation, and location-based information.
Service URL: policies.google.com (opens in a new window)